Hip, Foot & Ankle
Hip Fracture
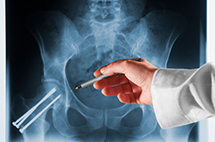 A hip fracture is a break in the top of the femur (thighbone) where the bone angles toward the hip joint. If the break occurs within two inches of the joint, it is called a femoral neck fracture. If it occurs between two and four inches from the joint, it is known as an intertrochanteric fracture. (A break further down the bone is classified as a broken femur rather than a broken hip.) Femoral neck fractures require more extensive surgery.
A hip fracture is a break in the top of the femur (thighbone) where the bone angles toward the hip joint. If the break occurs within two inches of the joint, it is called a femoral neck fracture. If it occurs between two and four inches from the joint, it is known as an intertrochanteric fracture. (A break further down the bone is classified as a broken femur rather than a broken hip.) Femoral neck fractures require more extensive surgery.
Hip fractures usually make it too painful for the person to stand. The leg may turn outward or shorten. They generally require hospitalization and surgical repair.
A person's risk for suffering a hip fracture increases if he or she is over 65, female, or small-boned; has a family history of hip fractures; has osteoporosis or low calcium, which leads to bone weakness; smokes or uses alcohol excessively; is physically or mentally impaired; or takes medications that cause weakness or dizziness. Hip fractures are a common and serious problem for the elderly, for whom a simple fall in the home may be enough to break the bone.
Hip Bursitis
Bursitis is the painful swelling of the bursae, fluid filled sacs on the cushion areas where tendons and muscles slide across bone. Specific to the hip is trochanteric bursitis (also known as greater trochanteric pain syndrome or GTPS), which refers to the bursa by the head of the femur. This shock absorbing sac can become agitated and swollen for unknown reasons or as a symptom of other issues such as gluteal tendon infections, uneven leg length or Iliotibial Band Syndrome. Steps can be taken to prevent bursitis by strengthening the core and hips through a moderate training program. Orthotic inserts for people with flat feet can also help.
The condition can be treated by:
- Rest
- NSAIDs or steroids to reduce swelling
- Physical therapy
- Surgical removal of the bursa (bursectomy)
Foot & Ankle
Plantar Fasciitis
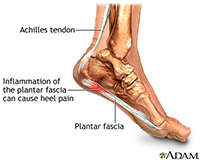 There is a ligament along the bottom of the foot called the plantar fascia that stretches from the heel to the base of the toes. If the ligament is forced to stretch beyond its limit, it may become inflamed and result in heel pain. This condition is called plantar fasciitis. Patients often complain of discomfort in the heel, the arch of the foot or the back of the leg when walking. The pain is usually worse when getting up after sitting or lying down.
There is a ligament along the bottom of the foot called the plantar fascia that stretches from the heel to the base of the toes. If the ligament is forced to stretch beyond its limit, it may become inflamed and result in heel pain. This condition is called plantar fasciitis. Patients often complain of discomfort in the heel, the arch of the foot or the back of the leg when walking. The pain is usually worse when getting up after sitting or lying down.
Bone spurs are a common complication of plantar fasciitis. These bony calcium growths on the bottom of the heel form where the plantar fascia pulls on the heel bone. Spurs don't usually cause pain themselves, but they are often a good indicator of the severity and age of the underlying problem.
Achilles Tendon Rupture
The Achilles tendon is the strong band of tissue that connects the calf muscle to the heel and helps you point your foot downward and push off as you walk. If stretched too far, the tendon can tear, causing severe pain in the ankle and lower leg that can make it difficult or even impossible to walk. An Achilles tendon rupture often occurs as a result of repeated stress on the tendon and may be partial or complete, depending on the severity of the injury.
After an Achilles tendon rupture, patients often experience severe pain and swelling, and are unable to walk normally or bend their foot. You may hear a popping or snapping sound as the rupture occurs. These symptoms are similar to those of other conditions, such as bursitis and tendonitis, so it is important to seek prompt medical attention in order to determine the correct diagnosis of your condition.
Treatment for an Achilles tendon rupture depends on the severity of the condition, but often requires surgery to repair the tendon and restore function to the foot. Less severe cases may only require a cast or walking boot for several weeks, although the risk of a recurring rupture is higher. Patients can help prevent an Achilles tendon injury by stretching the tendon and nearby muscles before participating in physical activity.
Ankle Sprain
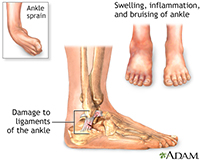 A sprain is a stretching or tearing of one or more ligaments, the tough fibrous bands that hold the ankle bones in place. Sprains can be caused by a sports injury, accident or stepping on an uneven surface. Symptoms may include pain, swelling, stiffness and bruising. There may be a popping sound when the ankle is moved. The ankle may be unstable or unable to hold weight.
A sprain is a stretching or tearing of one or more ligaments, the tough fibrous bands that hold the ankle bones in place. Sprains can be caused by a sports injury, accident or stepping on an uneven surface. Symptoms may include pain, swelling, stiffness and bruising. There may be a popping sound when the ankle is moved. The ankle may be unstable or unable to hold weight.
Your doctor can diagnose a sprain after performing a physical examination of the ankle and asking you questions about your symptoms and the injury. X-ray images may also be taken to confirm the diagnosis.
Ankle sprains can usually be treated through conservative methods such as resting the ankle, applying ice, wearing compression bandages and keeping the ankle elevated. Your doctor may also prescribe medication or recommend anti-inflammatory drugs to help reduce pain and swelling. Severe sprains may require avoiding walking for some time. Most sprains do not require surgery, and patients will be able to resume physical activity once the injury heals.
Ankle Fracture
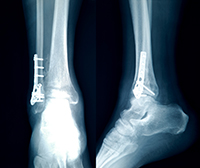 An ankle fracture is a common injury that involves a break in one or more of the bones that make up the ankle joint. Treatment for an ankle fracture can vary depending on the severity of the condition. While mild fractures may be treated through nonsurgical methods, more severe fractures may require surgery to realign the bones and ensure that they heal correctly.
An ankle fracture is a common injury that involves a break in one or more of the bones that make up the ankle joint. Treatment for an ankle fracture can vary depending on the severity of the condition. While mild fractures may be treated through nonsurgical methods, more severe fractures may require surgery to realign the bones and ensure that they heal correctly.
Open reduction internal fixation is a surgical technique that secures the bones in place with the help of screws, plates, wires, rods and pins that may or may not be removed from the ankle in the future. These tools allow the bones to heal properly, restoring function to the joint with no damage or discomfort to the patient.
![]() For more information about Our Services, or to schedule an appointment, please complete our online form or call 410-833-9300.
For more information about Our Services, or to schedule an appointment, please complete our online form or call 410-833-9300.
